Those with stroke and brain injuries learn to speak at Aphasia House.
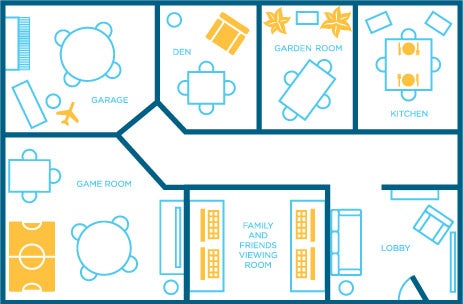
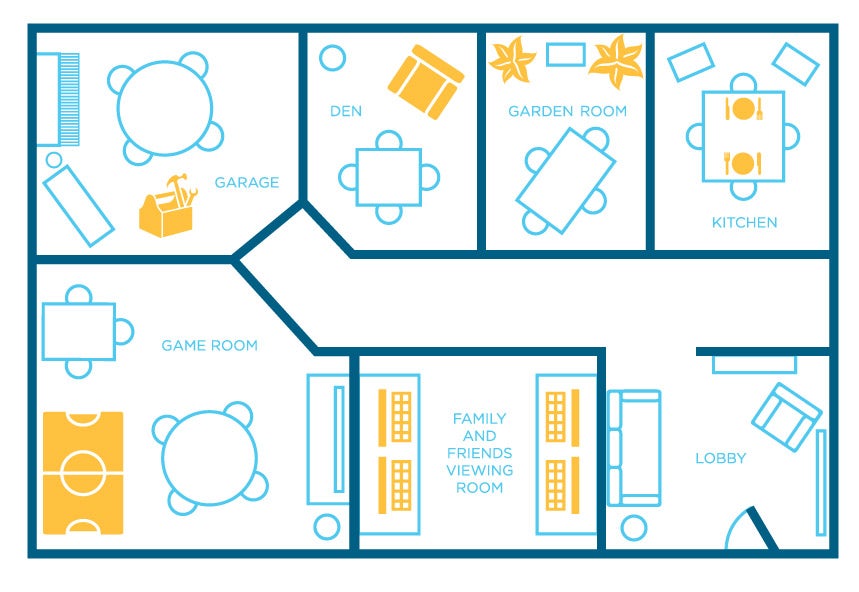
“This is the kitchen,” Dr. Janet Whiteside, chair of the Board of Clinical Educators at the UCF Communication Disorders Clinic, says with pride. “And this is the garage. The men love this room.” It’s as if she’s giving a tour of her own home, pointing out photographs on the wall (all taken by, and of, clients), knickknacks on the bookshelf, and a kitschy beach cruiser bicycle leaning against the wall.
“This is the fulfillment of a dream I first had in 1974,” she says. “I was at Vanderbilt University when I had the idea that people with communication disorders, like stroke survivors, would benefit from going through intensive therapy in a homelike setting. I knew it would be called Aphasia House.”
Today, Aphasia House is a reality, built out of a modest office suite at the Central Florida Research Park, and generating tremendous results.
According to the Mayo Clinic, “Aphasia typically occurs suddenly after a stroke or a head injury. But it can also come on gradually from a slowly growing brain tumor or a degenerative disease.” What makes it most devastating is that it doesn’t affect a person’s intellect. An individual with aphasia can usually process information fine; however, he or she may have difficulty comprehending language—and alarmingly—can’t formulate or articulate the words to express his or her thoughts, ideas, wants or needs.
Kelly Carroll, who is currently enrolled in the UCF Communication Sciences and Disorders master’s program, interned at Aphasia House. She recalls, “When all of a client’s methods of communication—gestures, writing, speaking—have failed, the feelings of frustration and defeat come through loud and clear. We could read our clients’ disappointment in their tone of voice, body language and facial expressions.”
Each Aphasic is Unique
The National Aphasia Association reports that more than 100,000 Americans acquire aphasia each year. Sadly, according to Whiteside, there are fewer than 10 intensive therapy clinics in the U.S., and none are based on her innovative homelike model, nor are any others affiliated with a university.
Whiteside insists that each of her clinicians focuses on one client (she eschews the word “patients” or just about anything that evokes a medical environment), creating a customized treatment program. “No two people with aphasia are the same,” Carroll notes, “and the individuals we worked with were all very unique, both in personality and aphasia.

As part of his therapy, one client used photography to share his feelings. When he passed away, his granddaughter donated his artwork, which now graces Aphasia House, and began volunteering her time.
Built as the result of an anonymous $25,000 donation, Aphasia House feels like a home, both in environment and in the level of care. Click the image to view it larger.

Dr. Janet Whiteside, College of Health and Public Affairs

To speed up results, clients receive one-on-one attention from familiar faces in homelike settings. Here, a client communicates with a student using an iPad application in the Aphasia House den.
It is the combination of intensive one-on-one treatment plans and the unique homelike setting that has attracted nationwide attention.
A Home for Aphasics From All Over the Country
It is the combination of intensive one-on-one treatment plans and the unique homelike setting that has attracted nationwide attention and helped build Aphasia House’s reputation.
“Many clients travel from all over the country to come here,” UCF graduate student Cyndel Barbarossa says. “My client was from Kansas, and his wife used Skype to watch his therapy sessions.”
Yet, while Aphasia House is attracting serious national attention—Arizona Rep. Gabrielle Giffords’ speech-language pathologist recently visited—Whiteside wants people to know that there is more to it than just pretty pictures and comfy couches. The environment has a therapeutic purpose.
“Environment really does enable one’s ability to communicate,” she says. Conversations happen more organically, and memories are triggered more easily when people are surrounded by familiar things.
UCF graduate student and former Aphasia House intern Kelly Keating, ’10, explains, “The person is going through all these changes. Their lives have been changed … by the stroke or brain trauma. Things they took for granted, such as speaking, they couldn’t do anymore. Other environments—doctors’ offices, hospitals, clinics—can be cold and sterile. But Aphasia House, with its family pictures, gardening tools and kitchen … gives a calming feeling. It’s less intimidating.”
Denette Schweikert can relate. An award-winning artist and successful businesswoman, Schweikert suffered a stroke last year. Since then, she has spent hours in the sterile rooms of hospitals and doctors’ offices, with their fluorescent lights, cold tile floors, and paper-covered exam tables. As she talks about her time at Aphasia House, however, she brightens. “The environment is what makes it,” she says. “The ladies are all so caring and concerned. We drink coffee and talk to different people. Your family can be there too, to watch and see what’s going on.”
The Environment is Comfortable, but the Treatment isn’t Easy
Aphasia House’s clients receive intensive therapy four days a week, four hours a day for six weeks. They work one-on-one with Whiteside and her team of clinicians, all UCF graduate students. But not all the work is done on site. At a nearby restaurant, clients face their fears—by ordering a meal. Communicating with family or sympathetic clinicians is one thing, but facing an impatient server adds a layer of stress. But this is the point, to return to living a normal life. And once this hurdle is cleared, when the meal is ordered and on its way, this sense of accomplishment often leads to more success.
Clinicians are also encouraged to use their imaginations to develop innovative therapeutic techniques. Carroll says, “We used the iPad quite frequently. I would preprogram the target sentences, and the client would use those as the stimuli for melodic intonation therapy, which requires the client to tap out the syllables of the phrase or sentence he or she wants to say.”
Keating, too, turned to technology in planning her client’s therapy. She made a video of just her mouth saying simple words and phrases. “Ball.” “Computer.” “Kitchen.” Her client watched the video intently, working hard to emulate the way Keating’s mouth and lips moved. Keating recalls with pride, “It worked.”
For client Schweikert, the entire approach worked. She completed her second, six-week session, and her clear, confident voice conveys true pride in her achievement. “I did a lot better than I ever thought I would. But it was about the fourth week when I said, ‘Oh my gosh!’ and realized that all of a sudden, I could talk again.”
That type of breakthrough is great, but it is only the beginning. Whiteside explains, “We are concerned with how the loss of language changes one’s ability to participate in life. The goal of Aphasia House isn’t simply to get people talking again. It is to get people working, spending time with friends, going bowling, baking with their grandchildren, tinkering with their cars. The goal is to get them living again.”
Now, Schweikert’s goal is to regain her fine motor skills so that she can paint again. And the confidence she has gained from her time at Aphasia House will certainly help her fulfill that goal.
But the clients aren’t the only ones changed by their experience here. “One thing Aphasia House taught me about patient care,” Barbarossa says, “is to be my client’s greatest listener. As a 23-year-old preparing to embark in the real world, I learned how to effectively communicate with adults, both with and without communication disorders.”
The impact that Aphasia House has had on so many people—clients, their families, Whiteside’s students and herself—is clearly something she takes great pride in. In ways she probably never could have anticipated when the idea first came to her almost 40 years ago, Whiteside has built a house where dreams really do come true. ✦
What is Aphasia?
Aphasia is an acquired communication disorder that impairs a person’s ability to process language, but does not affect intelligence. Aphasia impairs the ability to speak and understand others, and most people with aphasia experience difficulty reading and writing.
What Causes Aphasia?
The most common cause of aphasia is stroke (about 25 to 40 percent of stroke survivors acquire aphasia). It can also result from head injury, a brain tumor or other neurological causes.
How Common is Aphasia?
Aphasia affects about 1 million Americans, or one in 250 people—making it more common than Parkinson’s disease, cerebral palsy or muscular dystrophy.
Source: National Aphasia Association