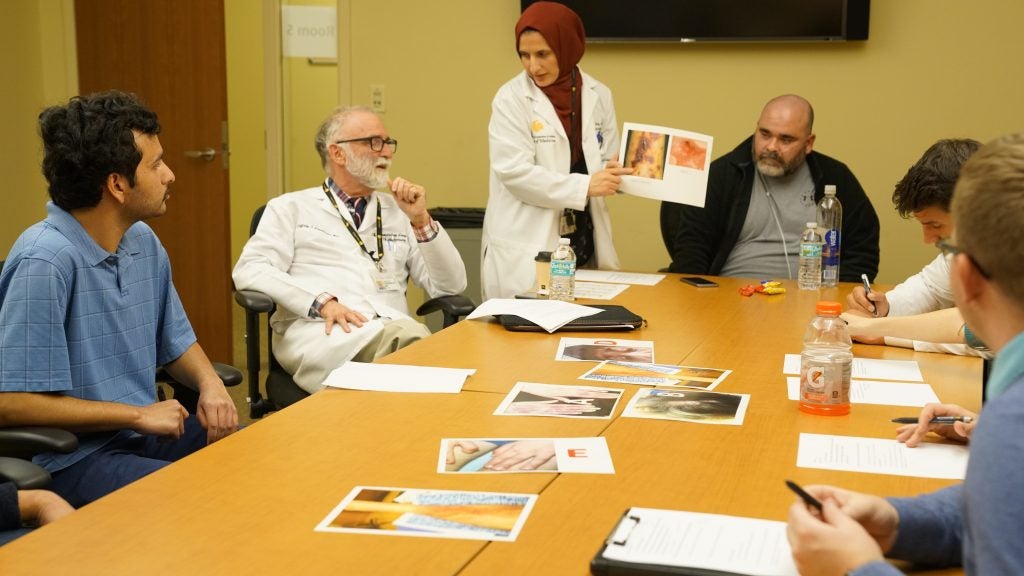
John McLees was a first-responder on Sept. 11 and today he suffers from lupus, rheumatoid arthritis and respiratory problems he attributes to the dust and fumes he inhaled protecting others. On January 15, McLees became a retired police officer-turned teacher as he volunteered to share his life and medical condition with second-year UCF medical students.
McLees and five other patients with rare autoimmune and skin diseases – such as lupus, scleroderma and psoriasis — spoke during the skin and musculoskeletal module directed by Shazia Bég, a rheumatologist at UCF Health and assistant professor of internal medicine.
“When my patients hear that I teach, they immediately ask about helping me with my classes as they want to educate others about these rare diseases,” says Bég, who treats five of the six volunteers.
“I am hoping when the students leave here today they will be able to diagnose this disease early.” – Roy Louden, UCF Health patient
“The diseases that I cover in my module are pretty rare, so my students get to talk to the patients and see these diseases that they may not ever see again. Just to hear the patients’ stories, see their symptoms and how they present with these illnesses really resonates better, as they can literally put a face to the disease.”
For Roy Louden, teaching others has become a way for him to cope with his illness. Louden suffers from scleroderma, an autoimmune rheumatic disease that affects approximately 300,000 Americans. He has been assisting Bég with her classes since 2012 and has a YouTube channel where he educates others about living with scleroderma. Now in the advanced stages of the disease, Louden’s symptoms are visible — skin tightening and muscle wasting in his limbs has caused his hands and wrists to bend inward. But in its early stages, the disease is difficult to diagnose. Louden says he volunteers to speak at the medical school because he wants to help future doctors recognize his disease’s early symptoms.
“A lot of scleroderma patients I’ve met online say they went undiagnosed for years because some doctors can’t recognize it or they don’t remember it from med school if they even learn about it,” Louden says. “So this is my way of helping, it’s my way of staying positive and making impact. I am hoping when the students leave here today they will be able to diagnose this disease early.”
During the exercise, organized by Bég and Jeff Greenwald, assistant professor of dermatology, students rotated through small roundtable sessions where they engaged with each patient. They did not know their patient’s disease but had about 15 minutes to review the patient’s history and see current symptoms to reach a diagnosis. They asked questions about symptoms, when they first appeared, and had patients show them photographs of previous skin lesions.
McLees, who served as a New York Police Department sergeant, says he finds fulfillment in helping medical students learn. “When I heard that Dr. Bég was a teacher, I volunteered to help her with her students in whatever way she needed,” McLees says. “It’s really rewarding for me knowing that I am helping to train the next generation of doctors, showing them a real life patient with these health issues which is beyond a textbook with pictures. And it’s more than just teaching them about the diseases, they are also learning to interview and engage with patients in a compassionate way.”
“It’s very easy to remember when you’re engaging with an actual patient and seeing the visible symptoms of diseases.” – Courtney Bell, UCF medical student
First and second-year students usually develop their interviewing and diagnosing skills by working with “standardized patients” – actors who pretend to have a medical condition. So for some, Bég’s session was their first experience interviewing a real patient with a disease.
“We learn about these diseases in class, but I felt way more engaged meeting the patients, and interviewing them to try to figure out what was wrong,” says medical student Daralys Lopez. “I feel like this was a nice change of pace to classes. I was also impacted by how positive and upbeat the patients were despite their illness.”
Second-year med student Courtney Bell says the interview sessions have made a lasting impression and have helped to cement the concepts she learned in class.
“You can teach us a hundred diseases in three weeks, we won’t remember everything. But it’s very easy to remember when you’re engaging with an actual patient and seeing the visible symptoms of diseases,” Bell says. “I’m not going to forget the time I met Mr. Louden or the 9-11 first responder with lupus. And this will definitely help us to remember these concepts years from now when patients come to us with these diseases.”