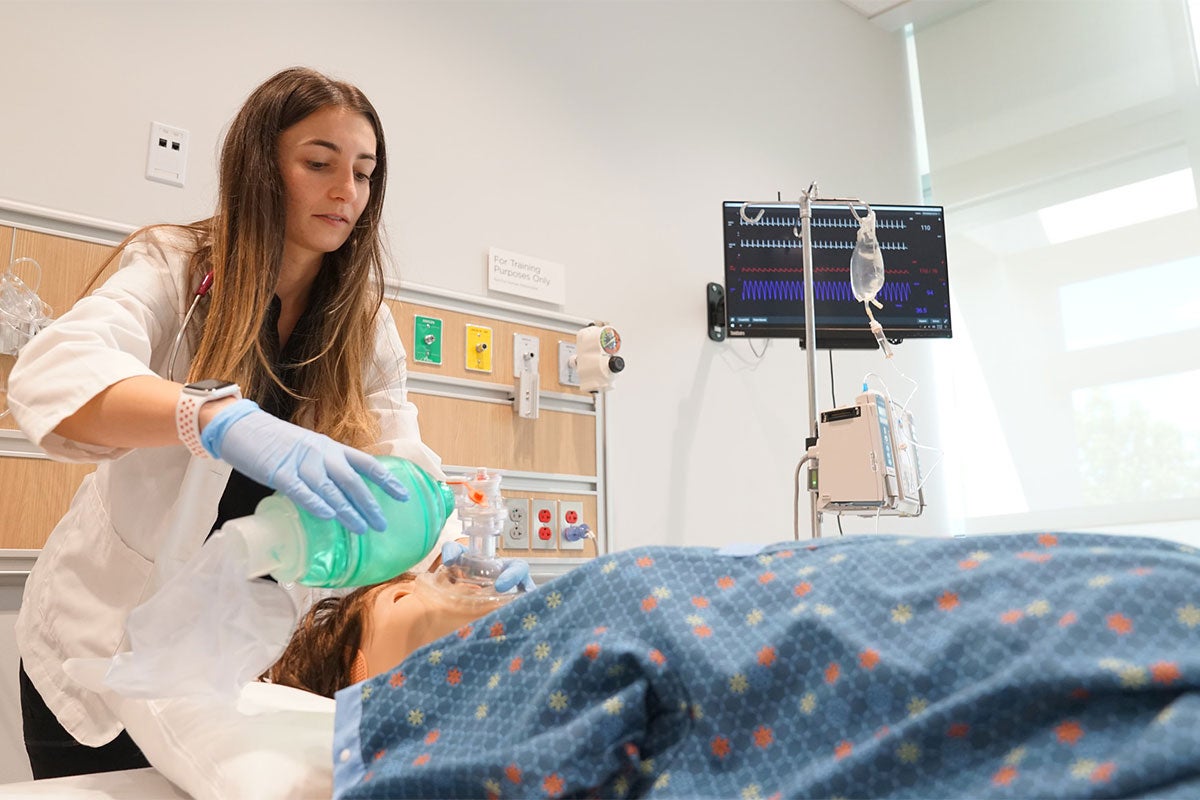
Students gathered around computerized manikins as monitors blared. The patient was non-responsive and in real time students had to re-position his bed, check his vitals and begin resuscitation as their instructor looked on.
This recent College of Medicine simulation module was designed to give rising third-year students a place to learn what they may encounter as they enter clerkships. At HCA Healthcare’s simulation training center at the UCF Lake Nona Cancer Center, students entered an environment that simulates a hospital setting — with interactive simulated patients operated from control rooms to mimic real-life interactions.
“It’s a big shift from text book learning to the clinic,” says Andrew Taitano, an Orlando VA Medical Center surgeon who helped create the transition-to-clerkship course. “This way we give students a foundation of knowledge in a safer environment so they can work through their nerves before getting to the hospitals.”
This is the first time in three years the course was taught in-person because of COVID-19 restrictions. And its curriculum was created and revised to address students’ feedback on additional training needs in actual patient-care settings.
“The course is to help reduce student anxiety and helps give them a review of everything from CPR to IV insertion under a doctor’s supervision,” says Analia Castiglioni, who leads the College of Medicine’s Clinical Skills and Simulation Center.
The training is unlike what they have received before because everything in the patients’ rooms — from defibrillators to oxygen and EKG machines — is designed to be fully functional, similar to what they will find in a hospital room. Basic skills, such as how to turn on a machine and know if it’s working properly or how to fit an oxygen mask on a patient, may sound simple but need to be practiced.
Taitano recently joined the Orlando VA and UCF after serving at the CW Bill Young (Bay Pines) VA Medical Center, where he was the director of the bariatric surgery program and taught UCF medical students. At the Orlando VA, he will oversee medical students in general surgery during their month-long clerkship rotations.
“I really get a lot of joy from teaching, it’s tremendously satisfying to see students progress in their surgery and technical skills,” he says.
Students say the simulation session was especially helpful because so much of their education has been virtual because of COVID-19.
“The experience was invaluable,” says med student Brittany Perry, who will begin her clerkship this summer. “The feeling of camaraderie among my classmates as we shift into a new phase of our training, listening to the real-world stories and advice from our dean, clerkship directors, and transitions facilitators, and experience in the SIM lab just inspires us to do our best and sets us up for success from day one.”
As part of his FIRE (Focused Inquiry and Research Experience) module, rising second-year medical student Ri Chen is working with his mentor, Nemours Children’s Hospital pediatrician Shiva Kalidindi, to research the effectiveness of this clerkship training. He helped design three surveys that participants will complete before and after the course to continue revising the curriculum based on real-world needs.
Chen attended the recent transition session and watched his peers tentatively handle the new procedures.
“All students have different clinical experiences,” he says. “Some have never done this before, so it’s helpful to go through the motions before the hospital setting. It’s fascinating and exciting to know I’ll be going through this in a year.”
The collaborative session included providers from UCF, HCA Healthcare, the Orlando VA and Nemours and is part of the medical school’s increased use of simulation.
“We are using simulation more to integrate into the curriculum so that there is more hand-on training,” says Castiglioni. “That means the students will be familiar with what alarms mean, how to respond and it will make a big difference for them to be able function as a medical team.”