
Models for Success
Spring 2020 | By Robert Stephens
On a Sunday evening, Jack Stubbs’ phone rings. He thinks about letting it go to voicemail until he notices who is calling: a doctor from Nemours Children’s Hospital. A small child with badly impacted teeth needs surgery right away, but it’s complicated, possibly life-threatening. The medical team looks to Stubbs for help.
Stubbs is not a doctor. As the director of the Prototype Development and 3D Print Lab (PD3D) at UCF, he’s basically a gadget guy. His demeanor is as casual as the jeans he wears to his office at Central Florida Research Park. Here, Stubbs shows what first appear to be toys. Behind him, the constant drone of printers creates a soothing backdrop of white noise.
“This is the cool stuff,” Stubbs says. What you see barely begins to convey what he means. Over here is a head small enough to be on an American Girl doll — except it’s more humanlike. Hey, isn’t that a heart? It’s remarkably realistic. Oh, and there’s a rib cage with slime around a kidney.
“That’s a patient-specific replica of a child’s midsection,” says Stubbs. “The green stuff [represents] the tumor. We don’t know the child’s name or where the family lives, but I’m guessing it’s a girl, about 5 years old.”
In other words, we’re looking at the closest depiction possible of a body part of an actual child. We’re also looking at her cancer.
“A tumor isn’t the nice, tidy lump you see in pictures. In real life it’s messy, and it makes the job of a physician challenging. That’s why these models are so valuable. We’re helping doctors save lives,” Stubb says.

To be able to look at a model of a tumor from all angles, without the restrictions of an image on a computer screen, is completely changing how we are planning complex surgery,” says Physician Craig Johnson, who is enterprise director of interventional radiology at Nemours Children’s Health System and chair of the department of radiology at Nemours Children’s Hospital in Orlando. (Photo by Nick Leyva ’15)
“A tumor isn’t the nice, tidy lump you see in pictures. In real life it’s messy, and it makes the job of a physician challenging. That’s why these models are so valuable. We’re helping doctors save lives.”Jack Stubbs
Physician Craig Johnson chairs the department of radiology at Nemours Children’s Health System. He sees the young lives that are at stake and talks with the families trying to cope. He also appreciates the importance of Stubbs’ contributions.
“The key to advancing medicine and saving lives is to combine the minds of doctors, clinicians and engineers,” says Johnson. “That’s why Jack’s patient-specific models are game changers. You have to remind yourself that each model is an exact replica, down to 0.1 millimeter of what is actually inside that child.”
The phone call Stubbs received on Sunday helps illustrate the lifesaving process. A doctor tells him about the patient’s teeth being buried deep among neurological tissues. Highly developed MRIs and CT scans are helpful only to a certain point.
“Can you help us?” the doctor asks.
This is what enticed Stubbs and Fluvio Lobo, principal research and development engineer at PD3D, to leave their lab at the University of Minnesota and take positions at UCF. Here, they have the opportunity to combine technology, healthcare and education to do something incredible — one precious life at a time.

At UCF’s PD3D lab in Central Florida Research Park, Director Jack Stubbs, Principal Research and Development Engineer Fluvio Lobo, Director of Generative Design Jim Inziello and artist Robert Sims ’19 collaborate with Nemours to produce the final 3D-printed surgical planning models. (Photo by Nick Leyva ’15)
A few hours after the phone call, Stubbs’ team receives images of the child’s skull. Then the magic happens. PD3D director of generative design Jim Inziello and researcher Robert Sims ’19 add color-textured surfaces and features that will allow the doctors to better visualize the focal points of the surgery. The information is fed into a Stratasys Polyjet J750 printer — one of the most advanced 3D printers of its kind, and one of the first to use FDA-approved software to develop anatomical models. Soon, a replica of the child’s jaw will be in Stubbs’ hands. He will deliver it to the physician, who in turn will use it with a team of neurologists, reconstructive surgeons and nurses. They will see the jaw and the buried teeth and the brain, not in pictures, but in the closest thing to real life. Then they will practice the surgery before the surgery.
“It takes out the guesswork, big-time,” says Johnson. “The surgeons can see everything the way they’ll see it when they open the actual body rather than on a two-dimensional flat-panel TV. Sometimes they’ll change their approach, maybe change an angle to remove a tumor and also save a kidney rather than taking it all out.”
It’s something Johnson could barely imagine when he and a colleague first saw a 3D printer at Best Buy in 2014 and thought, “What if?” The future seemed to arrive fast when Nemours partnered with the PD3D lab three years later. Their first case together provided the ultimate test.
“We had a teenager whose family had been told there was no way to treat a tumor that had grown to the size of a small basketball,” says Johnson. “The tumor was around too many of his organs, and it had blood vessels around it. Chemo wasn’t working. He had no more options.
The Nemours doctors weren’t sure how helpful a model from the PD3D lab would be.
But they practiced on the model prior to the surgery and strategized how to specifically and safely remove the tumor. The boy walked out of the hospital three days later.
“It’s been two years, and he’s had no recurrence of the cancer,” Johnson says.

Pushpak Patel, a radiology technologist, leads 3D printing services at Nemours and works with the hospital’s CT and MRI groups to make the right imaging for the models. (Photo by Nick Leyva ’15)
While Stubbs and Lobo don’t have direct contact with patients, they do hear the good news from the doctors. “Hearing that … it means a lot,” says Lobo.
Word has started to spread. The UCF team has provided patient-specific models for hospital teams as far away as Seattle and San Francisco. Lake Nona Medical City will present more opportunities as it grows. Stubbs does admit frustration about moving this technology out further and faster, even though the 3D-printed models are being used in 113 hospitals in North America and more than 250 worldwide.
“That isn’t enough. There are thousands of hospitals around the world,” he says, holding a replica of a rib cage. “This only costs $1,200 to print. We have an opportunity to change healthcare — to make it more affordable and to save lives.”
“This only costs $1,200 to print. We have an opportunity to change healthcare — to make it more affordable and to save lives.”Jack Stubbs
Hospitals, despite copious financial reserves, cannot realistically do what’s being done at UCF. It isn’t just a $400,000 3D printer. It’s literally a village, where expertise in computer science, mechanical engineering, biomedical sciences, psychology and architecture can make these tiny heads and hearts come to life.
“Art students are as important as anyone,” says Lobo. “They paint each model to look the way a doctor will see it in surgery. They don’t make it pretty — they make it realistic.”
Stubbs hands over a model of two conjoined heads, so small they both can be held in one palm. With this model, two lives could be saved.
“It’s hard to describe how motivating it is when we hear what we hear on the other side of this procedure,” says Johnson, referring to a child in post-op. “It’s more than a black and white image or a piece of plastic. It’s a living child.”
In the laid-back office at Research Park, a printer continues to hum. The model of the child’s impacted teeth should be ready later this afternoon. Stubbs will deliver it himself to the surgical team, who will be given the chance to see the nuances and angles they hadn’t seen previously. They will operate tomorrow.
“This is as real as it gets,” says Stubbs. “How cool is that?”
MODELS FOR SUCCESS

A clear plastic was used to create a model of 3-month-old conjoined twins to allow doctors to clearly see where their blood vessels are located. Craniopagus twins, those who share a skull but not a brain, is a rare phenomenon and separation surgery requires surgeons to navigate delicate networks of arteries and veins that can often be tangled.
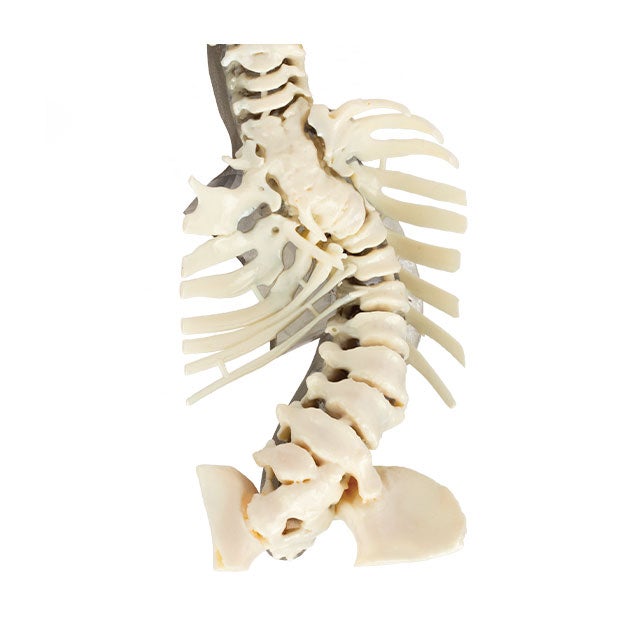
This model of an 8-year-old patient’s severe scoliosis allowed doctors to show and explain to the patient and his parents exactly how the child’s spine was curving. It also allowed surgeons to determine a surgical plan that would be almost impossible to visualize and plan using CT images alone.

The yellow object depicts a tumor within the abdomen of a 3-year-old patient. Surgeons used the model to determine how to remove the mass, which was growing between his kidneys (shown in dark red) and his pancreas (teal), while being sure to not rupture any of his veins (blue) or his arteries (orangish-red).

To help a 15-year-old patient better understand how a heart functions and how his particular condition affects it, doctors at Nemours Children’s Hospital used this model, which combines colors and labels to illustrate the patient’s anatomy. For example, the dark blue region in the front is a pulmonary artery, magenta is the right ventricle and yellow is the left ventricle.