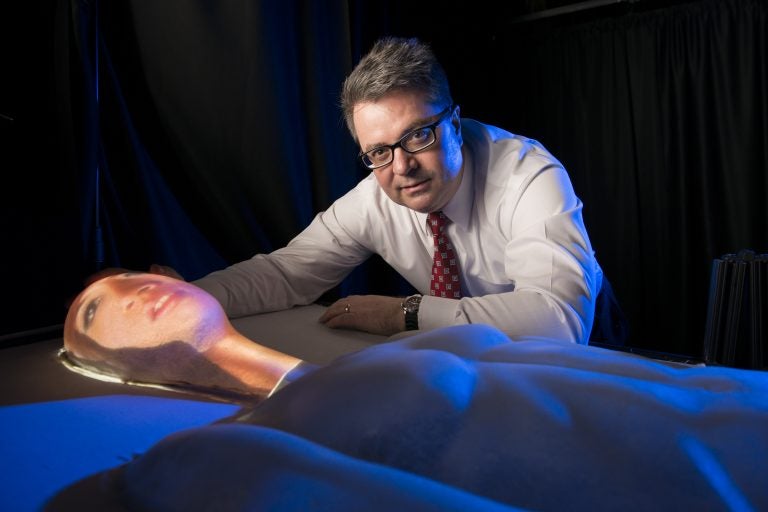
He can sense and respond to touch, look you in the eyes and exhibit real emotions. But this patent-pending simulated patient, developed by a team of UCF researchers, is not human.
“One of the unique aspects of this new tool is its ability to bring humanity to simulation,” said Gregory Welch, a computer scientist and engineer who designed and built the hardware with colleagues.
“A nursing student will be able to make emotional connections with this ‘patient’ that you can’t do with a rubber mannequin– and that is critical for nursing. Compassion and empathy are an important part of earning patient trust, facilitating care and ultimately, healing.”
This tool, called the physical-virtual patient bed or PVPB, combines the benefits of two existing health care simulation training technologies – the physicality of mannequins and the flexibility of virtual patients. The result is a “patient” that is able to talk, sweat, breathe, exhibit a pulse, feel warm or cold on various body parts, respond to touch by humans or medical instruments, and exhibit real human emotional complexity.
“One of the most challenging aspects of the project from a computer science standpoint is the touch sensing. It needs to detect someone touching the surface, figure out where on the body its being touched, tell the simulator what part of the body needs to react, and render pictures of it moving in a very fast and accurate way,” explained Welch. “For example, if you dragged your fingernail across your skin, it would leave a mark. That’s the kind of direct interaction we want to have.”
Also, unlike current high-fidelity simulation mannequins, the PVPB is able to change race, gender, ethnicity and visually apparent symptoms on the fly. This provides increased flexibility for faculty and researchers to design and execute simulated training.
“For nursing students, the PVPB will help bridge the gap of realism where static mannequins drop off,” said Laura Gonzalez, simulation coordinator and clinical assistant professor at the College of Nursing. “A more ‘human patient’ will foster students’ ability to be caregivers, provide enhanced learning capabilities in areas such as neurological symptom assessment, and overall more closely mimic real-life practice while still providing a safe, learning environment through simulation.”
Welch, the Florida Hospital Endowed Chair in Healthcare Simulation at the UCF College of Nursing, is currently in the first year of a three-year $894,431 grant from the National Science Foundation to develop and assess health care training on the PVPB. He and the team, which include co-investigators Gonzalez and Dr. Juan C. Cendán, professor of surgery at the UCF College of Medicine, expect to complete development and begin research using the tool by the end of 2017. Initially, the team will use the tool to gain new knowledge about patient behavioral and physiological cues and the associated student behavior.
The PVPB also has the ability to provide critical training for difficult-to-diagnose conditions, such as sepsis. “An experienced nurse has the ability to make a very rapid assessment of a patient’s condition by just looking at or talking to them,” said Welch. “We want to be able to capture some of these thought processes and use them to help train others. If we know a timely and accurate diagnosis involves observing two or three particular things, it is important that a simulator can present those things.”
Further immediate research opportunities for the PVPB are in pediatrics. Welch and the team are in the process of creating a smaller, transportable PVPB that can be used to simulate a toddler or infant. “Children behave and communicate differently than adults,” said Welch. “It is important to have training tools that are as close to real as they can be to help practitioners learn to diagnose and treat pediatric patients.”
“There are so many things we can study and do with this,” added Welch. “In the future, I see the PVPB as a potential new tool in the arsenal of training at simulation centers around the world.”