Mary Lou Sole pauses for a moment before allowing herself to go there. Back to the day in 1991 when she was flipping through a magazine and saw these words: University of Central Florida. The old days, you might say.
Over the past 40 years, UCF’s nursing program has graduated more than 11,000 alumni who have gone on to work in the White House, risen to the ranks of Chief Nursing Officers, and launched their own groundbreaking healthcare businesses.
“Honestly, I’d never heard of it,” she admits. Intrigued, Sole visited the little-known campus when she and her husband moved to Florida from San Antonio, Texas, where she taught in the University of Texas at Austin’s School of Nursing. On the eastern edge of Orlando, she saw an “intimate” department of nursing with 500 students and 17 faculty members. But during that tour, she sensed something much bigger than sheer numbers.
“There was this willingness to try new things,” says Sole, who would eventually go from curious visiting instructor to the Dean of UCF’s College of Nursing. “I knew right away it could be a very different kind of nursing program.”
One of those new things was nursing simulation, for which UCF this month received accreditation from the Society of Simulation in Healthcare and the Council for Accreditation of Healthcare Simulation Programs.
Over the past 40 years, UCF’s nursing program has graduated more than 11,000 alumni. They’ve moved on to work in the White House, risen to the ranks of Chief Nursing Officers, and launched their own groundbreaking healthcare businesses. But the résumés, just like the numbers, are not the core of what makes UCF’s College of Nursing stand out. To understand “different,” you have to see their education in action, in real time.
Healthcare by Total Immersion
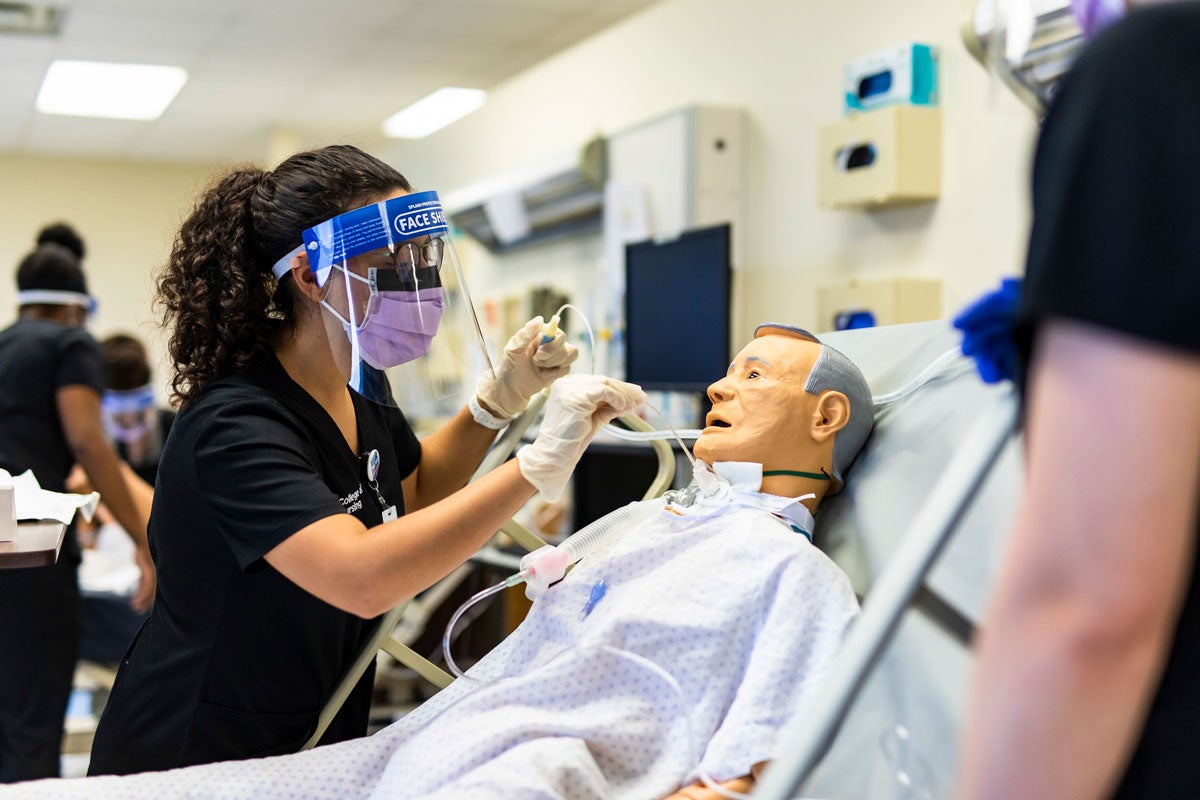
Step off the elevator and onto the 6th floor of University Tower in Central Florida Research Park. You’re no longer in a typical classroom setting. This is a hospital wing. There’s a nurse’s station, gurneys, IV stands, ultrasound machines and — during times when we’re not physical distancing as a result of a global pandemic — a healthcare team discussing rounds as well as patients in need of various types of care.
UCF’s Simulation, Technology, Innovation and Modeling (STIM) Center is as real as you can get without real consequences.
Earlier this spring before the campus closed, I visited that hospital wing just as medical chaos was about to ensue.
A young woman named Lauren is going into labor in an obstetrics (OB) suite. It’s a risky birth because Lauren’s medical history makes her a candidate for postpartum bleeding. The baby, Hunter, has a wide frame and seems to be experiencing shoulder dystocia (when the shoulders are too large for the birth canal). Hunter might have breathing problems, too.
Two nursing students enter the room, which is also filling with intensity. They introduce themselves and wash their hands. They’ve got this … hopefully.
We are witnessing healthcare by baptism — total immersion. The students are preparing for worst-case possibilities at UCF’s Simulation, Technology, Innovation and Modeling (STIM) Center. It’s a creative type of nursing education. It’s unpredictable. It’s as real as you can get without real consequences.
Both mother and baby are highly-sophisticated manikins, which can look similar to mannequins you see in a clothing store but are much more advanced and used in healthcare simulation training. For example, Lauren has a pulse. Her lungs and bowels make sounds. She actually goes through labor and gives birth to Hunter in this room. You’d never know from the serious mood on the 6th floor that all of the patients have been tailored by the engineering and computer science labs across the street in Central Florida Research Park. Each nursing student signs a contract before entering STIM training. The contract says, “Although this is not a human, I will treat it as if it were my own mother.”
The simulation is so well orchestrated, so professional, in many ways it’s more impactful than a literal hospital experience.
“We set it up so students provide the type of hands-on care that they might not have a chance to experience in hospital training,” says Laura Gonzalez, UCF’s director of simulation in the College of Nursing. “In labor and delivery, for example, a mom-to-be probably doesn’t want nursing students observing at the bedside. But here, the students have to work through it. They don’t know what’s going to happen until it happens.”
Just like real life.

A Hub of Healthcare Simulation Expertise
There’s a commotion around the corner in another patient room. It’s Greg Harrison. Mr. Harrison’s chart says he’s 51 years old, has no known allergies, and he came in for complications related to acid reflux. But something is starting to go wrong.
“We decided [simulation] is where healthcare education needed to go, and we wanted to be the leaders. So we hired internationally-recognized experts to create critical mass and momentum.”
— Dean Mary Lou Sole
“I feel queasy and can’t get comfortable,” Mr. Harrison says.
Two certified facilitators are in a control room down the hall, observing the nursing students on a TV monitor. One instructor has a headset and mouthpiece so she can be the eyes, ears and voice of Mr. Harrison.
“Tell me what else you’re feeling, Mr. Harrison,” says one student.
“It feels like butterflies in my chest, and I’m sweaty.”
As the students look at his chart and check his vital signs, Mr. Harrison suddenly goes into cardiac arrest.
A virtual Greg Harrison or a human Greg Harrison would be in good hands on this floor. The expertise is staggering. Doctors and nurses from UCF’s world-class healthcare partners provide feedback and sometimes participate in the simulations. And the faculty and staff are literally a who’s who in the field of simulation. Gonzalez, Desiree Díaz and Mindi Anderson were three of the first certified advanced healthcare simulation Educators (CHSE-A) in the world. Syretta Spears, the assistant director of UCF’s STIM Center, is one of the premier certified healthcare simulation operations specialists. Their presence has attracted the most sought-after simulation educators to the nursing program, and made it possible for UCF to be one of the only universities in the nation to offer a master’s degree and a graduate certificate in healthcare simulation.
“There was some debate a few years ago about whether we should go all-in with simulation,” says Sole. “We decided this is where healthcare education needed to go, and we wanted to be the leaders. So we hired internationally-recognized experts to create critical mass and momentum. The STIM Center on the 6th floor exemplifies our investment in people and resources.”
The student-to-facilitator ratio is typically never higher than four-to-one, better than many hospital internships. Patient rooms have ventilators, defibrillators, cabinets stocked with supplies, and six manikins that cost $45,000 to $65,000 apiece. The technology and the knowledge to apply it to healthcare education is so impressive that leaders from other major nursing schools come to the 6th floor to observe it in motion for themselves.
But UCF’s College of Nursing still has something that cannot be bought or touched. It’s what shaped the program when it opened in 1979 and attracted Sole, who was recently reappointed as dean, here in 1991.
“We’re nimble. What worked in the past for a certain type of care might not be the best approach now or in the future,” says Gonzalez. “We have the freedom to mix things up and expose our students to anything.”
And “anything” is underway at this moment.
A Better Way to Prepare Nurses
Uh-oh. A little boy has gone into respiratory failure in the room next to Mr. Harrison. His name is Paulie G. The facilitators in the observation center watch to see if the students notice Paulie G’s heart rate dropping to 60 beats per minute and how quickly they administer treatment.
“It is like getting on an airplane with a pilot who has only read a manual on how to fly. You want to know they have at least been in a simulator a few times. Isn’t healthcare just as consequential?”
— Assistant Professor Desiree Díaz
“It’s just like you find in the workforce,” says Gonzalez. “Always changing.”
In Mr. Harrison’s room, two other students have started CPR. They’re up against another obstacle you’ll never deal with in a classroom: It’s Mr. Orion, a close friend of Mr. Harrison.
Mr. Orion is a live volunteer, one of the “embedded participants” from the UCF community who comes in and adds another layer of realism to simulation. He’s basically an actor. Sometimes the participants are subtle. Sometimes they aren’t. One might play the role of a mother who goes hysterical over a child’s worsening condition. Or there could be a temperamental husband in the room with his sick wife.
Mr. Orion? He’s just a good friend of Mr. Harrison coming to chat. But he shouldn’t be in the room during cardiac arrest. A nurse needs to have the presence of mind to politely ask him to leave.
Over the course of these 60 minutes, you observe that UCF’s College of Nursing isn’t specifically a healthcare model and it isn’t a social-work model. It’s both — the blend of art and science and the wherewithal to sometimes show people the door.
When each simulation is over, the students and instructors will go into a debriefing room and replay on a monitor what just happened. They critique. They compliment. They cringe. They correct. It’s much better to learn from mistakes here on the 6th floor than out there.
“In a hospital, a first-year nurse might be asked, ‘Have you ever done this? No? Well we need you to try it now, on a live patient,’ ” says Díaz. “It is like getting on an airplane with a pilot who has only read a manual on how to fly. You want to know they have at least been in a simulator a few times. Isn’t healthcare just as consequential?”
Quite often the staff receives emails and calls from nurses in the field. They’re UCF graduates giving thanks. As in, “We had a risky medical situation yesterday and I knew what to do because of what we learned in simulation.”
But there’s another angle to it all. Simulation isn’t just vital signs and prescriptions and Mr. O’Rion leaving his walker in the doorway. Some of the most valuable lessons foreshadow encounters you might not think of in nursing until they happen.

Learning Empathy Through Simulation
No one knows this patient’s name. He doesn’t speak English and none of the nurses speak his language. He’s lost control of his temper and his bowels. The very best nurses might be able to put themselves in the shoes of the patient needing standard care or, more importantly, in the patient’s gown and bed. But this?
“Absolutely, you can learn empathy. To be a good nurse, you have to learn it, no matter the circumstances.”
— Assistant Professor Desiree Díaz
“Absolutely, you can learn empathy,” says Díaz. “To be a good nurse, you have to learn it, no matter the circumstances.”
Díaz became a simulation specialist with a research focus on healthcare disparities because it’s personal for her. In 1999, she was with her 5-year-old son on the French side of the island of Saint Martin when he was electrocuted. Díaz had trouble communicating with medical personnel because of the language barriers, even as her son’s hand melted to itself.
“I had all kinds of questions in that frantic moment, but there was no one to translate and interpret,” she remembers. “It happens more often than we might realize. So we need to make sure our students see nursing as much as a calling as it is a career. They cannot bring personal biases about people into care.”
The patient could be a teenage refugee or a traveler from another country. He wants his mom. It’s dark. His asthma starts to escalate. Do you wonder why the parents aren’t here, or do you comfort this boy as if you are his family?
A patient could be a transgender person who was in a car accident. Will you privately judge this person or treat them with the same love with which you’d treat your own brother or sister?
A patient could be an inmate from the county prison, making threats and yelling profanity at you. How do you protect yourself while also treating his internal bleeding as best as you can?
“Your preconceived ideas and thoughts about a patient will affect your actions as a caregiver,” says Díaz, “so we better figure out now how you’ll deal with your bias and fears in simulation. It is a safe place to be vulnerable.”
And what about that patient whose name you still don’t know? The one who has lost control of everything? Some lessons on empathy have to be learned more literally, without technology or Mr. Orion. In other words, there’s nothing like wearing a “poop bag” for two days to fully understand what it’s like for a patient who can’t help themselves.
“The perspective changes dramatically when a student feels almost exactly what a patient feels,” Díaz says.
As she speaks, Mr. Harrison is undergoing an operation of sorts.
Where Nursing Meets Engineering and Computer Science
Down the elevator and across the street from the STIM Center, Mr. Harrison is being recreated. The manikin is just like the current Mr. Harrison, but with facial expressions that can change in real time — a droop for a stroke, a grimace for pain, or a smile to say, “Thank you, that feels better.”
This is another differentiator for UCF’s College of Nursing: being in the same neighborhood with UCF’s world-renowned Institute for Simulation and Training.
This is another differentiator for UCF’s College of Nursing: being in the same neighborhood with UCF’s world-renowned Institute for Simulation and Training (IST). While the elite nursing simulation experts dream up a better Mr. Harrison, the engineering and computer science teams bring it to almost-life as a patented physical-virtual patient simulation.
“There aren’t a lot of layers between here and there,” says Gonzalez, referring to the interdisciplinary collaboration and to the distance between real and unreal.
Mary Lou Sole sensed the same nearly 30 years ago, a direct route from “never heard of it” to preeminence. But even prestige and leading-edge technology have never been the goal. For her, and for everyone within proximity of the 6th floor, all of the expertise and simulation and manikins with pulses point to one ultimate goal: Let’s make healthcare better, for real.